Pelvic Organ Prolapse

By Dr. David Qi, Advanced Urology
Updated 9:26 AM ET, Mon Jan 20, 2020
Pelvic Organ Prolapse Overview
A pelvic organ prolapse (POP) usually occurs in the pelvic floor muscles. The pelvic floor muscles are the muscles that form the hammock shape around your pelvic opening. The reason these muscles exist is to keep the pelvic organs in their place. These organs include the bladder, small intestine, rectum and the uterus. Pelvic organ prolapse is the descent of any one of these organs. It affects mainly the women who have given vaginal birth. When POP occurs, a woman may feel as though there is vaginal bulge, pressure on her vagina or lower abdomen, leading to mild or severe discomfort. Statistics show that most women will experience some form of POP after giving birth. However, the symptoms do not occur immediately after giving birth but rather appear years after delivery.
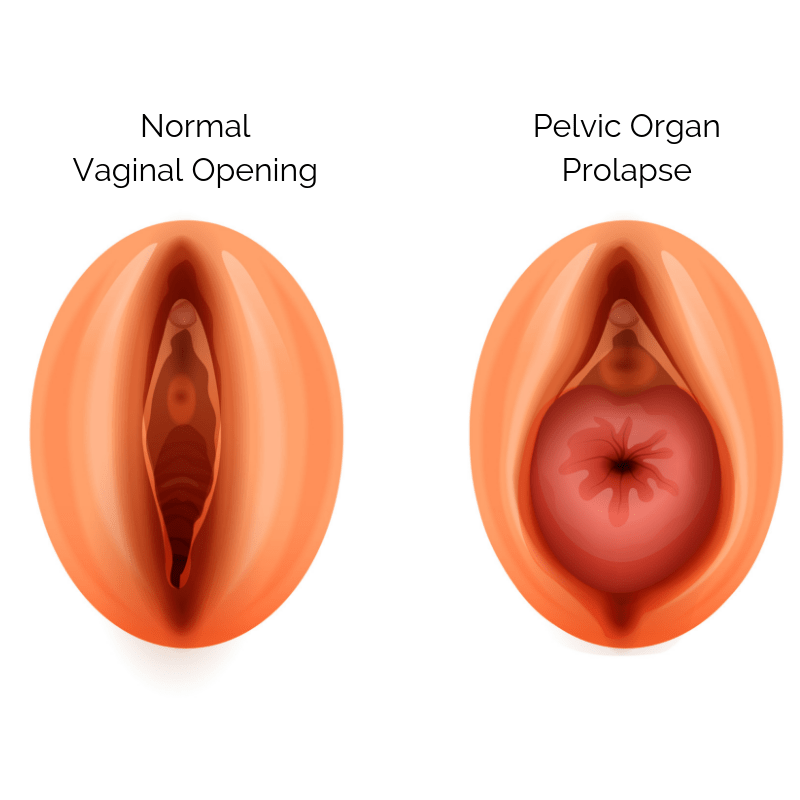
More About Pelvic Organ Prolapse
This condition is a result of damage, stretching, and weakening of the support structure of the female pelvis, which is composed of both muscles and ligaments. This can be a result of multiple factors including child birth, pelvic trauma, prior pelvic surgery (including hysterectomy), and abdominal/pelvic straining (heavy lifting, constipation, chronic coughing). With the damage, the organs gradually drop towards the lower pelvic region and come to settle on the upper wall of the vagina. This creates a sense of fullness and pressure. In some cases, this pressure can cause pain either when urinating or having sex. Postmenopausal women may also suffer from prolapse even if they have not given birth.
Causes and Risk Factors for Pelvic Organ Prolapse
Pelvic organ prolapse is associated with bodily changes that come with childbirth and/or age. If you are about to give birth or have given birth in the past, then you may be susceptible to the condition. There have also been studies that indicate the condition may also be hereditary. Generally, there are three main causes of pelvic organ prolapse:
- Childbirth – The strain that comes with vaginal childbirth can distend or damage the muscles that keep your organs in place leading to pelvic organ prolapse after childbirth.
- Age – As you age, your muscles may weaken and lose their ability to keep your organs in place.
- Hysterectomy – Surgical removal of the uterus can also lead to POP.Risk FactorsWhile risk factors associated with known causes of POP are ever-present, there are other risk factors that seem to contribute to the occurrence of POP. These can also affect women who have not given birth.They include:
- Obesity – If you are extremely overweight, the weight can push down on your organs and cause POP.
- A chronic cough – The pressure of coughing can weaken your abdominal muscles and lead to your organs descending.
- Constipation – Because of the pressure exerted when trying to relieve yourself, abdominal muscles may become overstretched and weakened.
- Because women’s estrogen levels are at much lower level during menopause as they are post-pregnancy, the chances of a pelvic organ prolapse occurring are raised during menopause. One of the reasons for this is because lower estrogen is directly correlated to lower collagen, a protein that is essential in keeping the pelvic tissues intact.
- Tumors – Any tumors in your pelvic area and especially on your pelvic organs can lead to POP.
How to Manage Pelvic Organ Prolapse
It is possible to prevent or manage POP by taking steps to strengthen your abdominal muscles and mitigate any risk factors associated with POP. While these steps are effective, they cannot eliminate the chances of POP occurring, especially after childbirth.
Here are some steps you can take to prevent or lower the chances of getting POP:
- Strengthen your pelvic muscles – This can be done by regularly performing Kegel exercises.
- Do sit-ups – Sit-ups strengthen your core muscles and may help prevent POP. It is important to note that POP involves smooth muscles (involuntary) while the muscles you exercise during sit-ups are skeletal muscles (voluntary).
- Manage constipation – If you have regular constipation, consider managing it to prevent straining your organ muscles and tissue. You can do this by eating plenty of high-fiber foods, drinking enough fluids, doing gentle exercises and taking stool softeners.
- Lose weight – As obesity has been linked to POP, losing weight can relieve the pressure the extra weight puts on your organs.
- Attend birthing classes – Birthing classes like Lamaze teach you how to tighten your core muscles and push during labor. This will help you know how to push and avoid straining your muscles.
When to See a Doctor in Atlanta for Pelvic Organ Prolapse
In most cases, women with pelvic organ prolapse have no symptoms. The condition will mostly be identified during a routine exam. However, in most women, the main sensation that proves to be bothersome is the bulge and pressure on the vagina. The other signs of Pelvic organ prolapse symptoms include:
- Pain in your pelvic region
- Pressure in your pelvic region even when your bladder is empty
- A sense that there is something falling out of the vagina
- A pulling or stretching sensation in your groin area
- Vaginal bulge or ball between the thighs
- Need to push on the bulge to urinate or defecate (splinting)
- Lower backache
- Pain during sexual intercourse
- Spotting or bleeding during your non-menstrual days
- Incontinence and frequent and sudden urges to urinate
- Constipation and other bowel movement problems
- If you need to sit in a certain way to relieve yourself
You may also visit the pelvic organ prolapse website( https://www.voicesforpfd.org/ )to view pelvic organ prolapse images and understand the condition better.
Pelvic Organ Prolapse: Diagnosis and Testing
A pelvic reconstructive surgeon will be able to perform tests and screenings that can evaluate thoroughly whether you have pelvic organ prolapse. But before any of these preliminary tests can be carried out, the doctor will first need to know all about your previous surgeries and medical history as well as any prior medical conditions and medications that you might be on. The doctor might need to examine your pelvic organs in order to get an idea of how strong your pelvic muscles are. This evaluation is essential in order to come up with a proper diagnosis.
How To Know When To Get Tested For Pelvic Organ Prolapse
While there are several pelvic organ prolapse treatments available, it is important that you get in touch with an experienced pelvic reconstructive surgeon as soon as possible in order to ensure best treatment. There may be dozens of questions racing through your head if you experience some of the symptoms of pelvic organ prolapse. If this is you, you may already be researching solutions online with queries like “pelvic organ prolapse testing near me.” While there are always certain questions that you should consider in order to reach the best decision regarding your health, you’ll need to factor in several elements such as the severity of the pelvic organ prolapse as well as how long the pain lasts.
The Most Common Tests for Pelvic Organ Prolapse
Here are some of the most common POP diagnostic tests.
Bladder Function Test
One of the most adverse effects of pelvic organ prolapse is that it can cause involuntary urine leakage. This is referred to as “incontinence” in medical terms. The bladder function test will prove incredibly helpful for the doctor to evaluate the current condition of your bladder. Additionally, it also provides information regarding the other pelvic organs near the bladder and how well they’re functioning.
Ultrasound
An Ultrasound uses sound waves in order to get both external and internal images of your pelvic organs. This is extremely helpful in letting the doctor know if multiple organs have been dislocated. This, in turn, leads to a better pelvic organ prolapse diagnosis.
MRI
An MRI is a superior option compared to an Ultrasound because it can create a 3D image of the organs as well as the muscle around the pelvic region. It allows the doctor to more accurately evaluate whether a person needs pelvic organ prolapse treatment.
Treatment Options for Pelvic Organ Prolapse
Medications and Supplements for Pelvic Organ Prolapse
For the women experiencing pelvic organ prolapse discomfort, vaginal Estrogen might prove helpful in alleviating some of it. One of the reasons for prolapse in the first place is that during menopause, a lot of women experience an extremely critical drop in estrogen levels. This lack of estrogen causes the pelvic muscles to weaken significantly and lead to vaginal dryness. There are no approved supplements or medications that can treat pelvic organ prolapse.
Pessary for Pelvic Organ Prolapse
A pessary (soft, harmless supporting implement) can be used to alleviate some of the symptoms of the prolapse. Pessaries are generally miniature silicone devices that are placed internally among the pelvic muscles to prevent further pelvic organ prolapse pain. These also prevent any more damage to the pelvic muscles before the surgery can be performed.
However, if these have complications or patient doesn’t like them then pelvic organ prolapse surgery is the next option.
Surgery (Natural tissue repairs, Native tissue repairs using patients own tissues, Non-mesh surgery, Mesh surgery)
Pelvic organ prolapse surgical treatment differs from person to person based on each patient’s medical history, pre-existing conditions and any medications that they’re taking. It also depends on the experience and training of the pelvic reconstructive surgeon. Here at Advanced Urology there are several options that the surgeons might choose from. Each option is designed with specific factors and individual patient needs in mind. Rest assured, the surgeons will choose the best one capable of solving your problems without causing any side effects.
Surgical Treatments for Pelvic Organ Prolapse in Atlanta
NON-MESH PELVIC ORGAN PROLAPSE SURGERY/ NATURAL TISSUE REPAIR/NATIVE TISSUE REPAIR USING PATIENT’S OWN TISSUES (Vaginal surgery or abdominal or Robotic surgery)
These surgeries are mainly done through the vagina as it offers natural orifice surgery with no incisions externally and offer the fastest and quickest recovery. There is NO MESH used during these surgeries. Very high level of research has repeatedly shown that NON-MESH Vaginal surgeries for POP, if done by a properly trained and experienced pelvic reconstructive surgeon, will have better surgical outcomes with minimal complications compared to when using Vaginal MESH kits (https://www.voicesforpfd.org/pelvic-organ-prolapse/mesh-information/) These surgeries include the following options which are often done in combinations at the same time:
Sacrospinous Ligament Fixation
In this surgery the top of the vagina is most often suspended to a woman’s own pelvic ligament called the sacrospinous ligaments. This will restore the top of the vagina to its normal location. This is a very specialized surgery and is only done by an experienced pelvic reconstructive surgeon.
Vaginal hysterectomy and uterosacral ligament suspension prolapse Surgery
This is for women who have uterine prolapse and don’t wish to have any more children. In this the surgeon removes the uterus altogether and uses patient’s own pelvic ligaments called Uterosacral ligaments to restore the normal anatomy and to repair the prolapse. Please note that simply doing the hysterectomy or removing the uterus alone for the prolapse is not enough and will inevitably lead to failure and recurrence of the prolapse.
Uterine sparing surgeries
This is for women who have uterine prolapse and wish to keep their uterus. In this uterus is lifted and suspended to one of the ligaments of the body either uterosacral ligaments or sacrospinous ligaments.
Anterior Prolapse Surgery or cystocele repair
This is the surgery that is performed when there is a bladder drop also known as cystocele. In this the connective tissue between the bladder and the vagina is secured in order to restore the bladder to its original position using the patient’s own tissue or cadaveric tissue grafts.
Though it is rare, if there are traces of any excess tissues, the surgeon will remove them. If there is an indication that you might have urinary incontinence, then a sling may be placed under your urethra to prevent any involuntary urine leakage.
Posterior Prolapse Surgery or rectocele repair:
This is the surgery that is performed when there is a rectal drop also known as rectocele. During this surgery the connective tissue between the vaginal muscles and the rectum is repaired and the rectum is restored to its normal position.
Obliterative Procedures
For those women who do not desire to maintain sexual function, an obliterative procedure may be the quickest and least risky method to correct prolapse. Obliterative operations correct prolapse by narrowing and shortening the vagina. These procedures support the pelvic organs with the patient’s own pelvic muscles in such a way as to make the vagina too small to accommodate a penis for sexual intercourse.
The skin overlying the vaginal bulge is removed, and the front and back walls of the vagina are sewn to each other. A woman who has undergone this surgery will look the same on the outside of her genital area and she will be able to have bowel movements and urinate normally. Her ability to have an orgasm with clitoral stimulation is similar to before her surgery.
There are two main types of obliterative surgery:
- Partial (colpocleisis).
- Complete (colpectomy).
Both are very effective and durable in correcting prolapse. Prior surgeries often influence which procedure is offered to women. The benefit of obliterative surgery is that it is very durable, does not involve the risks of graft materials, tends to be less invasive and therefore is associated with a quicker recovery.
Vaginal mesh kit surgeries: There has been an FDA warning to use these vaginal mesh kits with caution. Pelvic reconstructive surgeons here at Advanced Urology do not offer any vaginal mesh surgeries for pelvic organ prolapse for that reason (Click here to read the FDA warning).
Even though we have extensive experience in helping women who have had vaginal mesh complications.
Abdominal Mesh surgery for Pelvic Organ Prolapse:
Sacro-colpopexy: This procedure utilizes a piece of polypropylene mesh to lift the vagina and attach it to your tail bone. This is most commonly performed using the Robotic technology these days. Note that this mesh is used through the abdomen or belly and not through the vagina and is relatively safer.
If you’re considering a procedure for POP, call Advanced Urology in Atlanta today at 404-238-7186 to learn more about treatment options and make an appointment.
RELATED ARTICLES
OUR VALUES
Our mission is to better human lives through personalized healthcare and innovation.
We are committed to providing compassionate and extraordinary care by acting with attention, joy and authenticity.
We advance healthcare by aligning patients, providers and payers.
We aim to lead the way by way of innovation, excellence and the drive to change and make a lasting difference.
Patient experience is our top priority. We show this by operating with integrity, listening, and building trust with our patients and one another.
We are committed to teamwork, family spirit and embracing each other’s resourcefulness, resilience and dedication.


