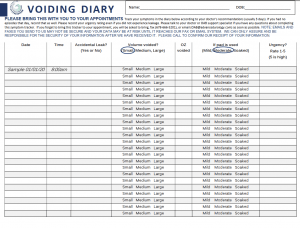
OVERACTIVE BLADDER
WHAT IS OVERACTIVE BLADDER (OAB)?
Having an overactive bladder (OAB) prevents you from controlling when and how often you urinate. You may experience unexpected small or large leaks or use the bathroom very frequently. The following are four symptoms of OAB, which may occur on a daily basis or may come and go unpredictably:
- Urgency of Urination: Feeling a sudden urge to urinate that is difficult to control
- Frequency of Urination: Urinating frequently, usually 8 or more times in 24 hours
- Nocturia: Waking up 2 or more times at night to urinate.
- Urge Incontinence: Involuntarily leakage after an urgent need to urinate.
ADVANCED STATISTICS
PHASES OF THE OAB PATIENT EMPOWERMENT PROGRAM
PHASE 1: ASSESSMENT / LIFESTYLE MODIFICATIONS

Depending on your symptoms, your provider may order testing to determine the severity of your OAB. Some common painless tests and what they tell us are…
- Urinalysis: A sample of urine is collected to check for abnormalities in the urine.
- Uroflow: You may be asked to urinate into a device that will measure the volume and speed of urination
- Post-Void Residual (PVR): After urinating, a quick ultrasound scan is performed to see what amount of urine is left in the bladder.
Renal Ultrasound
A renal ultrasound is a painless test that uses sound waves to visualize the bladder and other parts of the urinary tract. This test allows the urologist to look at the prostate (men), bladder, ureters, and kidneys. The test may be ordered to evaluate the history of blood in the urine (hematuria), anatomical structures of the urinary tract system, prostate size for male patients, and bladder wall abnormalities.
Cystoscopy
A cystoscopy is a painless diagnostic procedure performed with IV anesthesia in our Ambulatory Surgery Center (ASC) with anesthesia that uses a tiny camera to look at the urethra and bladder. The cystoscopy allows your urologist to check your urethra and bladder for narrow areas called strictures, abnormal growths, and other problems. This test may be ordered to evaluate the history of blood in the urine (hematuria), bladder pain, obstructive symptoms like straining or weak urinary stream, incontinence (Urine Leakage), and enlarged prostate (men)
Urodynamics Study
A urodynamics study (UDS) is a painless series of tests often performed with valium in the office that allow your doctor to look at how well your bladder, urinary sphincter, and urethra work. The tests help the doctor learn about any voiding or storing urine problems you may have. This test may be ordered if you report urine leakage, frequent urination, painful urination, a bladder that does not empty all the way, problems starting a urine stream, intermittent or a weak urinary stream, or nocturia.
Urocuff (For Men Only)
The UroCuff is a small cuff (like a blood pressure cuff) on the penis that can be utilized to non-invasively and painlessly measure urine flow rate and bladder pressure, as well as aid in the diagnosis of voiding disorders. This test may be ordered if you report urine leakage, uncontrollable urge to urinate, nocturia, frequent urination, intermittent or a weak urinary stream.
DIET
Eat a vitamin-rich diet. Vitamin C from fruits and vegetables (not a supplement) is associated with decreased urinary urgency. Water should be the majority of what you drink in a day (6-8 cups a day or 2 liters). Be sure to spread out your liquid intake throughout the day. Avoid known irritants such as carbonation, caffeine, and alcohol.
WEIGHT LOSS
Weight loss can significantly improve OAB symptoms. Losing weight will ease the stress on your bladder.
PELVIC FLOOR PHYSICAL THERAPY
Train your bladder by performing exercises to relax muscles around the bladder and go to the bathroom at scheduled times. Pelvic floor therapy exercises called Kegels help reduce leakage when you cough, sneeze, and laugh. The muscle you relax to urinate is called the sphincter. Relax the sphincter and then tighten the sphincter for ten seconds. Repeat this 30x daily.
PHASE 2: MEDICATION
There are two types of medications that can help relax the bladder: anticholinergics and beta-3 adrenergic agonist. These medications can help to relieve symptoms of overactive bladder and reduce episodes of urge incontinence. Not all patients are candidates for medications, so talk to your doctor about potential side effects. If your prescription is not covered by insurance, please ask your pharmacist what medications would be covered in place of it and give us a call back.
PHASE 3: LONG TERM SOLUTIONS

Depending on your personally identified goal, your provider will collaborate with you on a personalized treatment plan. Our clinical team, including your Personal Navigator, will guide you through your OAB care and will help you find the right solution for YOU.
Nerve Testing
The nerve testing also referred to as peripheral nerve evaluation (PNE) is typically used to evaluate bladder control problems. It is a temporary test where a small lead is placed just under the skin. This lead connects to an external neurostimulator (ENS) that you wear. Most patients report this as painless. For approximately 2-5 days (depending on physician guidance) you will complete a voiding diary that will be compared to a baseline (established by using a voiding diary prior to the evaluation). If successful, you should notice improvement fairly quickly.
Interstim
This therapy fixes the root cause of bladder dysfunction by targeting the nerves that control your bladder to help it function normally again. With this therapy, you may experience fewer trips to the bathroom, fewer accidents, and more confidence as you get back to the activities you enjoy. This is a long term solution and most patients are able to stop their medications.
- 84% satisfaction among those who use it
- 76% of people achieved success at 6 months compared to 49% who used medications
Botox
BOTOX® is a prescription medicine that is injected into the bladder muscle to temporarily treat OAB symptoms when oral medication does not work well enough or cannot be taken.
- The majority of patients receiving BOTOX® had at least a 50% reduction of daily leakage episodes
- Many of these patients reduced their leakage episodes by 75%
- Botox lasts 3-6 months and has to be repeated to maintain its effect
YOUR PERSONAL PATIENT NAVIGATOR
We go a step beyond the routine standard of care by offering a complimentary OAB Navigator Service. Your personal Navigator will contact you regularly to:
- Help you understand your diagnosis.
- Coordinate communication between you and your provider
- Facilitate scheduling treatments
- Guide you through the steps toward improvement in your OAB symptoms and meeting your personal goals